When I first wrote about COVID-19 a couple of weeks ago it was on the horizon but had not arrived with any intensity. The major concern at that time was that the virus would surge in and overwhelm our Health Care System. Canada has had an advantage over countries that had been bombed by this infection already in that we could see it coming and take action to avoid it. Social distancing was advised early. Public Health measures and planning were put in place.
In Kingston, Ontario, where I live, we have been fortunate to have been able to keep the “curve” pretty flat. Our community of about 215,000 people has only had 53 documented cases of COVID-19 with 36 of those people having recovered. As of April 10 we have not had any COVID-related deaths and only two people are currently in hospital being treated for COVID-19 specifically. Some of this is just good luck. But the community has certainly embraced the principles of social distancing responsibly. Other factors that may have helped are that the local university and college has closed up and many students have gone home. We have no tourists. Clinics are treating their patients “virtually” rather than in face-to-face visits. We have passed the 14 day risk period from returning spring break or winter snowbird travellers who have isolated themselves to protect the rest of us. Congratulations Kingston, it’s working for you right now.
There has been a partial flattening in other parts of Canada, too, but we are yet to reach the predicted peak later this week. Deaths from COVID will rise across Canada for the next couple of weeks. There is a 2-3 week lag between the number of new cases and the number of deaths because deaths don’t occur immediately when the diagnosis is made.
Is there a story behind these numbers that we have to consider? How reliable are these statistics? How do they compare to other countries or communities?
We have to bear in mind that the numbers are only for confirmed cases of the infection. People who have had milder symptoms or even no symptoms at all are not included in these figures. This means that the rate of infection in the community is certainly much greater than the numbers presented and that we must continue our social distancing practices both to protect ourselves and to protect others.
How can we actually compare how we are doing? Hospitalizations and deaths are figures that are more reliable and a reflection of what is happening in the community in general. About 10% of those who are infected will require additional medical care and are more apt to be tested and identified. We can look at those cases to determine the overall prevalence in the community. Death rates attributed to COVID-19 are also an indicator of how widespread the illness is. The consensus is now that COVID had about a 1% death rate. This does vary from one demographic or population to another but the affect of the virus on the community can be ascertained by looking at the death rate figures. Because population numbers from one country to another vary, I have been watching the deaths per million population number to get a sense of how comparisons can be made.
According to the Worldometer statistics up to April 10, Canada currently has had an attributed COVID death per million of our population of 15. For the USA this is 57 deaths per million. For Italy it is a terrible 312. Italy’s high rate is in part because they were taken by surprise when the infection arrived and their health care system was submerged quickly. This means that many people who might have benefited from more intensive care were unable to get it and subsequently died. There may be other factors like population density, a higher older population and more families with multiple generations living in the same household that influenced this as well. This disastrous result is particularly what we have been trying to avoid by “flattening the curve” and Canada has had the advantage of a bit of time to prepare and take precautions earlier than Italy.
We also have to be aware that this pandemic, although global, tends to be presenting unevenly in scattered epidemic areas, like New York City or Milan or even Toronto for example. So numbers might be drastically different from one locale to another.
The down side of being in the lower numbers right now is that this curve has not been erased but is only being flattened – stretched out so to speak. Because we have a lower prevalence in Kingston, we remain more vulnerable as we don’t have a significant proportion of people with naturally acquired immunity and immunization is yet a year away at least. The question is how will this unfold over the upcoming months? If we let up on our social distancing will it lead to a surge later that is hard to deal with? How can we gradually return to a more normal society and when will that happen? Will children be back in school in June? In September? When will people who have been laid off get back to work? How long will we be asked not to go for coffee or dinner with friends or family? When will I be able to go to a movie or a theatre event? When will travel restrictions be loosened up?
No one has answers to any of these questions yet. For the time being those of us who live in Kingston need to be glad that we have dodged this bullet and that we are currently able to sustain a reliably functioning health care system and not be overwhelmed with unmanageable numbers of seriously ill COVID patients or COVID deaths. But we are stuck in this holding pattern for the near future and maybe several more weeks or even months.
Before it is all over we will, unfortunately, lose many lives to this infection. But with time, it will subside. More people will acquire natural immunity from infections that don’t present severely. We will get more intensive testing to identify and aggressively trace and isolate specific people with symptoms and their close contacts. We could even identify those who have no symptoms but are infectious in order to limit contagion. We will get a quick test to identify people who are immune. I hope that we will also get some medical management to help manage the more severely ill patients, possibly reducing the need for intensive care and ventilation. And the final success will come when we eventually have immunization.
In the meantime, we must stay the course because for now, it is working, Kingston.
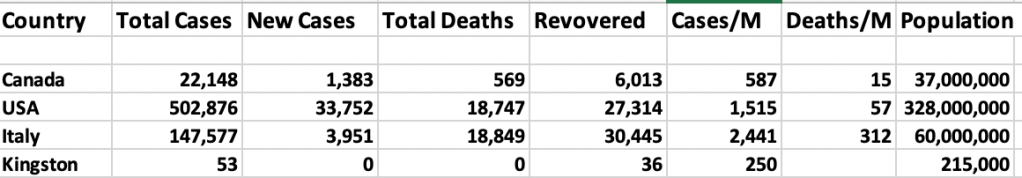
If you want more numbers, here are some figures from Worldometer and the KLFA Public Health Unit as of the end of yesterday, April 10, 2020. These figures change by the hour.

John A Geddes MSc MD CCFP
Kingston, Canada
